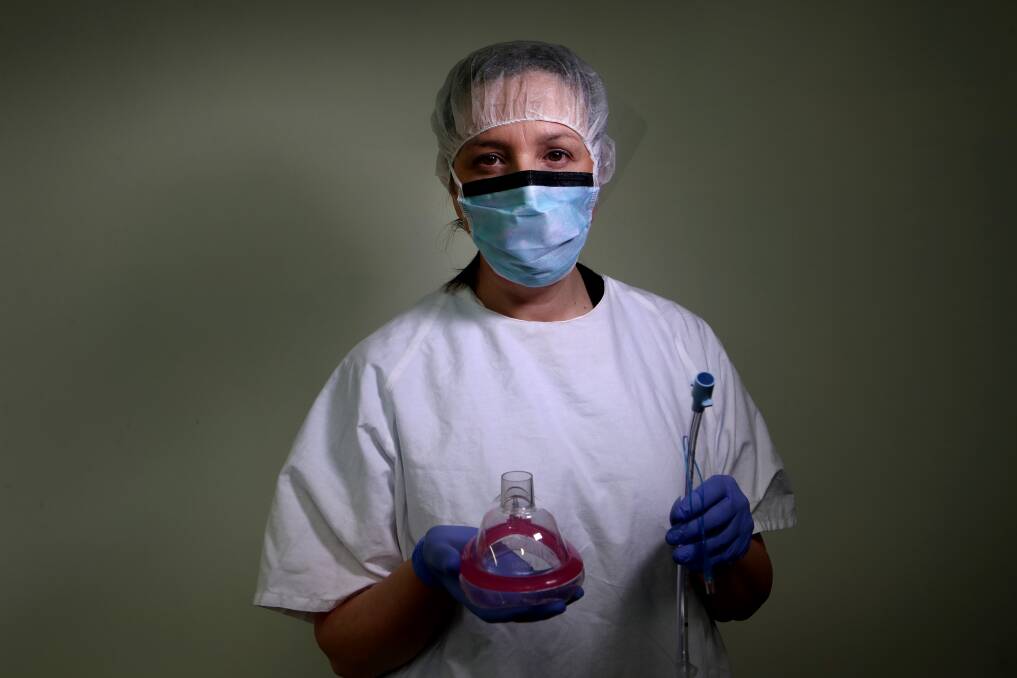
Dr Tanya Selak's three small children no longer rush to give her a kiss and hug as she walks in the door of their Bulli home after a long day in surgery.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
They know they must wait until the Wollongong anaesthetist takes off her scrubs and sets them aside for laundering - separately from the family wash; removes her shoes and bags them until her next shift; and steps into the shower to rinse off every evidence of her day in Wollongong Hospital's operating theatres.
For Dr Selak - and others in her speciality around the globe - has one of the riskiest jobs during the COVID crisis.
Tasked with intubating the most critically ill COVID patients, the process of placing the breathing tube through their mouths and down into their lungs causes the virus to become airborne, or 'aerosolised'. At that crucial time - when the anaesthetist's face hovers just centimeters from a patient's mouth - there is the highest risk for droplet exposure.
For Dr Selak, the COVID threat makes an inherently risky procedure that much more so.
"Some patients infected with COVID become so critically ill that they are no longer able to breathe safely on their own, because they're so tired as the infection is taking control of their body and can no longer support that vital function," Dr Selak said. "That's when we have to take over their breathing for them, by connecting them to a ventilator.
"In order to do that we need to give them medication - to put them in an 'induced coma' - and then place the breathing tube into their lungs to connect them to the ventilator. It places us at quite a unique risk - the patients are often short of breath and coughing, and the virus gets aerosolised leaving little bits of virus hanging in the air.
"We've had to take their mask off for the procedure and we are very physically close to them, putting our fingers and instruments into their mouths, with our faces close to theirs. It goes against the notion of social distancing."
Not that Dr Selak would hesitate to help those in dire need. Even though she's seen colleagues in the UK contract the virus. Even though she's already had to take measures to protect her family, and has earmarked a spare room to self-isolate in her home should the number of critical patients' skyrocket. It's what she was trained to do.

"Throughout your medical training you know you come to work no matter what - everything else is secondary," she said. "You miss weddings, funerals, Easter and Christmas celebrations - you miss most of your 20s! But you also know you must protect yourself and your colleagues - if you are sick, you can't look after other people."
A few weeks ago, Dr Selak worried that Australian hospitals - including Wollongong - would by now be inundated with those critical cases - that the COVID-19 'curve' would have followed the trajectory of other countries like Italy, the UK and US.
Yet she's been encouraged by the stablising of cases in the nation and the Illawarra Shoalhaven Local Health District; and by the changes made at major hospitals like Wollongong to cope with any surge that may come.
There's currently 114 confirmed cases in the local health district, with two patients being cared for at Wollongong and one at Shoalhaven Hospital.
"Compared to three weeks ago I feel a lot more encouraged by the numbers - back then we were on the steep part of the curve with case numbers doubling in Australia every three days," Dr Selak said.
"There had been no significant isolation measures instituted by the government - borders were still open, people were coming into the country with no checks, the Prime Minister was only started to talk about limiting gatherings to 500 people. There were no signs we were taking measures to flatten the curve.
"Then all of a sudden sweeping measures were introduced to quarantine, to self-isolate, to shut down bars and restaurants which caused the curve to flatten. And locally, at Wollongong Hospital, changes have taken place to stop non-essential elective surgery, to create dedicated COVID wards and intensive care units, to restrict visitors and screen everyone on entry."
Dr Selak said staff had pulled together during the COVID threat: "From the screeners at the front, the meal service team, security, wardspeople, the executive, the cleaners, the clinical staff - everyone has risen to the challenge and shown kindness, even when worried themselves".
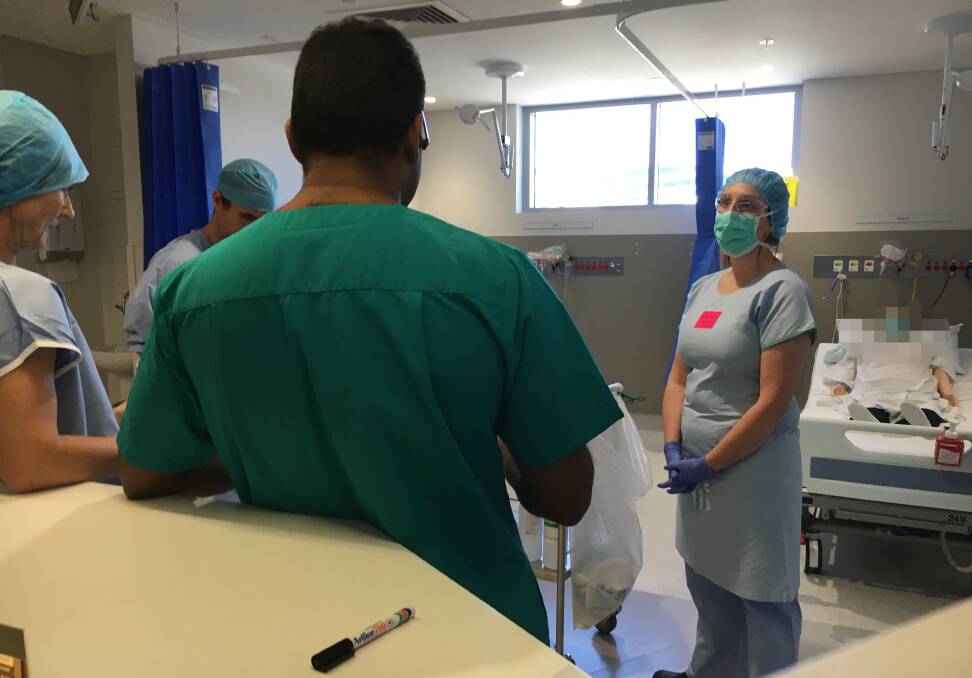
More could be done by governments, Dr Selak said, including expanding testing - where now it's limited to overseas travellers and those in contact with confirmed cases. There's enough protective gear at the moment, she added, but more needs to be done globally to reduce shortages.
Dr Selak was born in New Zealand where she attended medical school ahead of a stint working in the UK, before settling with her husband in Bulli where she's been for 13 years.
She's the first anaesthetist in Wollongong to be elected to the governing body of the Australian and New Zealand College of Anaesthetists, and is affiliated with the Illawarra Health and Medical Research Institute.
As well she's passionate about the use of social media to promote dissemination of health information - she co-hosts a podcast called Med Ed Stuff N Nonsense, and shares her experiences on Twitter (@GongGasGirl).
"Through my network of Twitter colleagues, I'm able to get instant cutting-edge medical knowledge from experts all over the world," she said. "I can draw on the vast experience of countries that have dealt with SARS, who are now dealing with the COVID-19 crisis.
"Normally you get that knowledge from medical journals that are peer reviewed - but we can't wait for that knowledge on COVID-19 to come in three to six months, we need it now."
If you're looking to stay up to date on COVID-19, sign up for our twice-daily digest here.

